A medical breakthrough made headlines in March but behind it was a story far bigger than the procedure itself… a patient who helped make it possible.
Western Cape, South Africa (16 April 2026) – After nine surgeries and years of setbacks, Martin Horn found himself staring at the same question again… what now? But this time, instead of another operation, he went looking for answers himself and what he found would change more than just his own story.
Last month, we shared the remarkable breakthrough when doctors in Cape Town successfully used cryoablation to treat recurrent cancer locally for the first time. At the time, it was a powerful medical milestone. Now, we have the full story… and it begins with the patient who refused to stop searching and the conversation that helped turn a possibility into a life-changing procedure.
For more than a decade, Martin had been navigating the exhausting cycle of diagnosis, treatment, recovery… and then recurrence.
“In 2012, I was diagnosed with papillary thyroid carcinoma, and first I had a partial thyroidectomy, then, after recurrence a few years later, a full thyroidectomy plus an oral radioactive iodine treatment. However, regular recurrences continued and in total I had nine surgeries on my neck over 12 years,” he says.
The very first of those surgeries came at a cost, severing a nerve to one of his vocal cords and permanently altering the pitch of his voice… a daily reminder of everything he had already endured. When recent tests revealed yet another small tumour growing dangerously close to his windpipe, the usual path forward simply wasn’t an option anymore.
“More surgery was not considered a good option for me. So, I started researching for myself what could be done,” he explains.
That decision, to take ownership of the search, became the turning point.
Martin’s deep dive into international medical research led him to cryoablation, a minimally invasive technique that uses extreme cold to destroy cancerous tissue. It wasn’t widely available locally for a case like his, especially given how close the tumour was to his trachea, but the more he read, the more convinced he became that this could be the answer.
“I discovered a 2023 US research paper with 10 papillary thyroid cancer patients in a very similar situation to mine, where cryoablation showed a significant success rate. I showed this study to my own oncologist to ask if we could explore this for me.”
“We didn’t know whether anyone in SA could perform this minimally invasive cryoablation so close to my trachea. I learned that cryoablation is gaining ground for treating certain breast cancers in Johannesburg, however the location of my tumour required a different set of sub-specialised expertise, and it was beginning to look as though travelling overseas for the procedure was my only option. It would, however, be considerably more expensive for me, as my medical scheme would likely not cover the costs.”
Martin connected with Dr Gercois Human, an interventional radiologist at Netcare University of Cape Town Private Academic Hospital, whose advanced international training placed him among a small group of specialists capable of performing this kind of intricate, image-guided procedure. Working alongside Dr Dale Creamer and the Cape Town Interventional Radiology team, they realised that what Martin had found wasn’t just possible… it was something they could do right here in South Africa.
“The considerable build-up of scar tissue from previous surgeries meant that it would be extremely difficult for surgeons to distinguish a tumour of this size, and traditional surgery so close to the trachea comes with additional risks. Essentially, surgical options for this patient had been exhausted when he turned to us for assistance,” Dr Human explains.
Interventional radiology offers a very different approach. Using real-time imaging, specialists can guide needles and instruments through the body with precision, reaching tumours without the need for open surgery. In cryoablation, the tumour and a small margin around it are frozen, effectively destroying the cancer cells while minimising trauma to surrounding tissue.
“Through interventional radiology, cryoablation freezes the tumour and a small margin of tissue around it to destroy the cancer. Overseas, this has been used to treat this type of cancer, but in South Africa, it was quite novel. Historically, interventional radiologists who trained internationally in procedures such as this did not return to practise in South Africa,” says Dr Human.
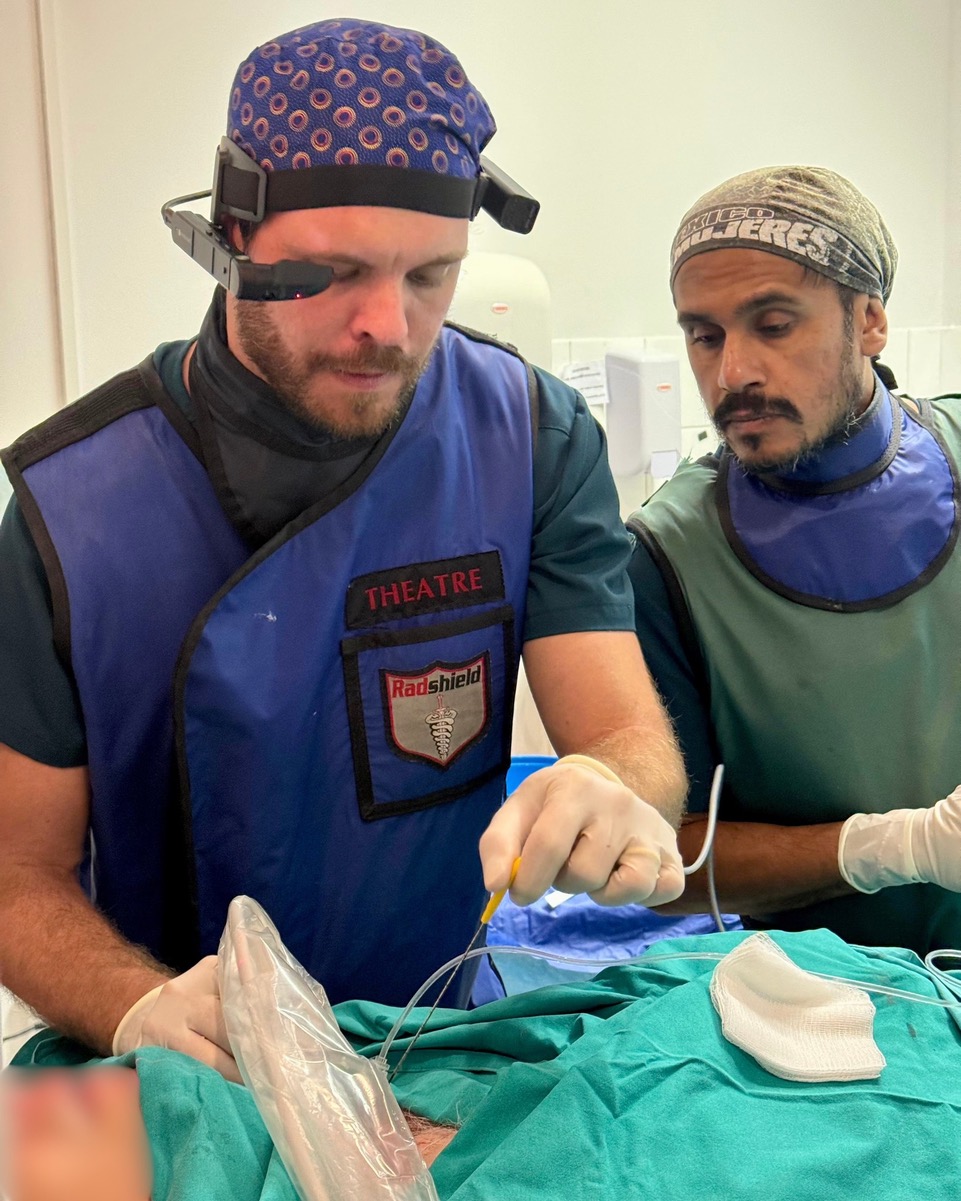
What made this possible wasn’t just skill but collaboration. The Cape Town team remains closely connected to global experts, including mentors in Canada who shared insights ahead of the procedure, ensuring that the approach was informed by years of international experience.
“Our Canadian mentors shared valuable insights before this procedure, and this ongoing collaboration ensures our patients benefit from years of collective experience,” Dr Human adds.
For Martin, the experience was almost surreal when compared to everything he had been through before.
“I was conscious, although sedated for the procedure and I drifted off to awaken back in the ward with only a small puncture in my neck.”
“This was worlds away from the experience of surgeries I have had before. I was able to return home the same day, and the next day I was back to my normal life. I’ll have regular check-ups with my oncologist to monitor my progress, but I want others who may be in a similar situation to mine to know that these options are now available in our country.”
Dr Human is clear that interventional radiology is not a one-size-fits-all solution, but its role is expanding quickly, opening doors across multiple areas of medicine.
“We aim to strengthen the availability of world-class cancer treatment options and minimally invasive procedures locally. These skills are scarce in South Africa, and to address this, Dr Jateel Kassim has joined our team as the first interventional radiology fellow in South Africa,” he says.
What started as one man’s search has become something far bigger than a single case. It’s opened a door, not just for patients like Martin, but for the future of cancer care in South Africa.



Ahh that’s beautiful!! I must admit I was hoping to read that they’d made a breakthrough using my son. He had a very confusing cancer journey and donated his body to Wits for cancer research when he passed in June last year in the hopes that they can figure out what was different, what went wrong, and to help prevent others from going through what he went through. Another factor in his decision was the utterly amazing CARE, like real actual I-truly-give-a-damn care, that he had from his oncologist at Charlotte Maxeke. Doctor Molepo will always hold a special place in my heart for the way he did his absolute best to keep my boy alive. My son and his doc are my heroes. Proper Legends. RIP my Bradley.